Introduction
One in eight women will be diagnosed with breast cancer in their lifetime. The earlier the cancer is detected, the better the survival chances. Since its widespread clinical deployment in the early 1990s, screening mammography has reduced the mortality rate for breast cancer by 39%. However, this approach cannot detect all tumours, and cannot recognize benign lesions from real tumours. Because the blood is in contact with every organ, including the breast, many people have tried to detect breast cancer with a simple blood test. However, considering the size of a tumor (especially before diagnosis) and the volume of blood, the clues are highly diluted, and current technologies have failed to reliably detect breast cancer in a droplet of blood.
Our Work
We are developing a novel technology that can simultaneously measure hundreds of different proteins associated with cancer in the blood with unrivalled accuracy. The technology will be exquisitely sensitive, inexpensive, and simple to use. We will use it to establish a molecular portrait - or fingerprint - of proteins in the blood for a large number of healthy women and cancer patients, and identify the molecular signatures of breast cancer. A successful outcome will thus produce a simple-to-use test to diagnose cancer using a droplet of blood and that could be performed at a physician’s office. The technology developed during this project will also become an attractive tool to study other cancer types, in terms of diagnosis in addition to prognosis and prediction of therapy efficiency.
Impact
The development of this technology will allow the identification of a molecular signature of breast cancer in blood. Then, the same easy-to-use and low-cost technology could be easily adapted as a rapid and noninvasive blood test in the physician's office to screen patients for breast cancer. It could be use as a standalone diagnosis test, or in combination to mammography, especially for women with dense breast for whom mammography is poorly efficient. This test should reduce mortality from breast cancer by a better and earlier detection. Thanks to the flexibility of this technology, it will be easy to perform similar study and come up with a similar test for all other types of cancer.
At the Micro & Nano Bioengineering Lab, we focus on identifying specific biomarkers in the blood that allow us to diagnose and detect various disease states. Biomarkers can include any measurable molecule that may indicate the presence of a particular disease, one such example being protein concentration. To make these measurements, we use a new technology that allows us to perform multiple measurements in small amounts of samples, the antibody colocalization microarray (ACM). Using a robotic pin spotter, we deposit tiny spots of antibodies, which are immune-system molecules that very specifically recognize proteins of interest. Using enzyme-linked immunosorbent assay (ELISA), we can detect hundreds of different proteins that can give a picture of the disease state.
First, a robotic pin-spotter delivers very small droplets of 'capture antibodies' (cAbs) specific to one type of protein biomarker. Each chip has 16 arrays of hundreds of these capture antibodies. These antibodies recognize and bind to specific proteins in your blood.
We add your processed blood sample on top of the capture antibodies. The floating dots are proteins in your blood that will bind to the capture antibodies.
Our machine prints a second round of small liquid spots that line up with the original spots. The new spots contain detection antibodies, which will also recognize and bind to specific proteins in your blood. Using this colocalization technique makes our method very sensitive and reliable because it is less prone to give false positive signals than other technologies.
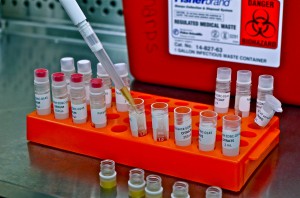
After collecting your blood, we transport it back to the lab where we centrifuge it down in order to separate the cells from the plasma. The plasma is the component of blood that contains the proteins that we will be measuring during our analysis. After centrifuging the tubes, we collect the plasma by pipetting it into various cryovials. As you probably remember, we collected multiple tubes of blood from each participant. Each tube contains different additives, and therefore the resulting plasma can be used for various applications. Each tube is aliquoted into its own colour coordinated set of cryovials.
The plasma aliquots are stored on dry ice for the day to keep them cool. At the end of the day, all of the cryovials are moved into storage in our liquid nitrogen tank. This keeps the samples extremely cold in order to preserve them until they can be used in the analysis phase of the study.
Investigators
Dr. David
Juncker
Associate Professor
Dept. of Biomedical Engineering,
McGill University
Biomedical engineering, microfluidics, nanotechnology and biomarker discovery
Dr. Sarkis
Meterissian
Professor
Dept. of Oncology; Surgery
McGill University
Director of the Cedars Breast Clinic at the MUHC
Collaborators
Dr. Morag
Park
Professor, Dept. of Biochemistry, McGill University
Director, Rosalind and Morris Goodman Cancer Centre
Dr. Benoît
Mesurolle
Associate Professor, Dept. of Radiology, McGill University
Radiologist,
Cedar Breast Clinic
Clinical Team
SARAH
BIENENSTOCK
Clinical Research Nurse, Phlebotomist, McGill University
NAOMI
BEZANSON
Clinical Research Nurse, Phlebotomist, McGill University
Amélie
Rivet
Clinical Research Assistant,
McGill University
Research Team
Dr. Karen
Gambaro
Research Associate, Study Coordinator
Dept. of Biomedical Engineering, McGill University
Pammy Lo
Research Assistant, Lab Manager
Dept. of Biomedical Engineering, McGill University
Veronique
Laforte
PhD Candidate, McGill University
Amanda
Marino
Undergraduate Volunteer
Axelle
Vallet
Visiting Student 2015,
École Polytechnique Fédérale de Lausanne
Jack
Mouhanna
Undergraduate Volunteer,
McGill University
Victoria
Kuta
Visiting Student 2014,
Queen's University